3 Ways to Reshape How You Communicate About Benefits with Millennials
Communicating the benefit needs amongst generations and can cause confusion when keeping up with the satisfaction of your younger employees. Ensure millennial happiness with these tips on their unique benefit standards.
As two millennials ourselves, we know what most people think about Generation Y. Many use terms like “techy,” “entitled” and maybe even “lazy” to describe our generation.
But, the reality is today’s millennials are more global, civic-minded and, though you may not expect it,financially conscious than any other generation. And, according to the Pew Research Center, we now represent 35 percent of today’s workforce.
Millennials are also now getting married and starting families. And yes, purchasing more benefits products through their employers as a result.
As we millennials grow up, it’s important to reconsider how you communicate with us about benefits—because it’s a lot different than how you’ve communicated with other employees in the past.
For example, consider your Gen X and Baby Boomer employees for a moment. When you communicate about benefits with them, it’s relatively straightforward. You probably use tools like email, in-person meetings, flyers and newsletters. And messaging probably revolves around safety, reducing risk and explaining the finer points of the benefits themselves.
But when you’re talking about benefits to millennials, things should be a little different. We’re more digitally fluent than other generations. We’re demanding more flexibility—in our work and family lives. And, we’re increasingly cost-conscious.
It’s a different approach. And, we want to talk about three key ways you can start to reshape how talk with millennials more effectively when it comes to benefits:
For millennials, it’s all about the emotion and sense of responsibility. One of the most interesting findings we’ve picked up over the last few years when communicating with millennials has been to focus messaging on making an emotional connection. Highlight the peace of mind benefits will provide. Discuss the fact that purchasing benefits like disability, life and critical illness insurance through their employer is the right, and responsible, thing to do.
In a recent survey conducted on behalf of Trustmark Voluntary Benefit Solutions “providing peace of mind” was the number one reason millennials gave for why they enrolled in key benefit areas. While this was true across all generations in the study, millennials chose “it’s the responsible thing to do” more than others as a secondary reason for purchase. That emotional connection tied in with responsibility is absolutely key when talking to this demographic.
Millennial stereotypes don’t apply. If you’re communicating with millennials, most people would think digital technologies like text messages and social media would be the way to go. However, that’s not the case. According to Trustmark research, millennials listed “meeting in person” and “calling a representative” as their top preferred channels for communicating during enrollment periods—followed by digital communications channels. Surprising, right? It probably shouldn’t be, given millennials’ desire for more personalization in multiple facets of their lives.
Value, convenience and high-level messaging are key. Through our research, we found that millennials react favorably to messaging around value and convenience—so be sure to hit on those points throughout the enrollment process. For instance, explain why coverage is needed or why an employer-paid policy is not enough. Talk about benefit policy costs in comparison to other low-cost items, like a daily cup of coffee. Discuss the value of employer contributions—and what those contributions can mean to millennials’ bottom lines. Also, make sure to share the convenience and ease of payroll deductions; how their employer is simplifying things by making the deduction and payment for them.
Finally, remember, when it comes to benefits, millennials aren’t as concerned about the details of their insurance plans. They want to understand the basics—what’s covered, how much it costs, and why they might consider a specific offering over another. Resist the urge to focus on the fine print, and keep messaging at the higher levels.
Magic number 3
One more thing that may help reshape your approach to communicating with millennials: The number three. That’s the minimum number of times you should be communicating with millennials during your enrollment process. Our research found that employees remembered and appreciated benefits more when they saw three or more distinct communications. In fact, 72 percent of employees who received three types of benefits communication rate themselves “likely” or “very likely” to recommend their employer based specifically on their benefits program.
Does that help give you some ideas for how to reshape your approach to communicating with millennials about benefits? Overall, just make sure to remember that we millennials are looking for personal and professional offerings from our employers that are unique to us—including benefits. And be sure you’re ready to talk with millennials using the right messaging, the right tools and the right cadence to ensure success.
SOURCE:
Dahlinger, M and Moser, C (27 June 2018) " 3 ways to reshape how you communicate about benefits with millennials" [Web Blog Post]. Retrieved from https://www.benefitspro.com/2018/06/27/3-ways-to-reshape-how-you-communicate-about-benefi/
Lack Of Insurance Exposes Blind Spots In Vision Care
Vision problems are typically not life threatening but can impact the success of your everyday life. Vision care is a significant benefit that could change the lives of many families.
Every day, a school bus drops off as many as 45 children at a community eye clinic on Chicago’s South Side. Many of them are referred to the clinic after failing vision screenings at their public schools.
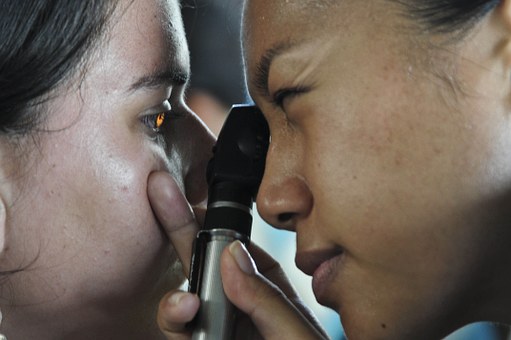
Clinicians and students from the Illinois College of Optometry give the children comprehensive eye exams, which feature refraction tests to determine a correct prescription for eyeglasses and dilation of their pupils to examine their eyes, including the optic nerve and retina.
No family pays out-of-pocket for the exam. The program bills insurance if the children have coverage, but about a third are uninsured. Operated in partnership with Chicago public schools, the program annually serves up to 7,000 children from birth through high school.
“Many of the kids we’re serving fall through the cracks,” said Dr. Sandra Block, a professor of optometry at the Illinois College of Optometry and medical director of the school-based vision clinics program. Many are low-income Hispanic and African-American children whose parents may not speak English or are immigrants who are not in the country legally.
Falling through the cracks is not an uncommon problem when it comes to vision care. According to a 2016 report from the National Academies of Sciences, Engineering and Medicine, as many as 16 million people in the United States have undiagnosed or uncorrected “refractive” errors that could be fixed with eyeglasses, contact lenses or surgery. And while insurance coverage for eye exams and corrective lenses clearly has improved, significant gaps remain.
The national academies’ report noted that impaired vision affects how people experience their world, including normal communication and social activities, independence and mobility. Not seeing clearly can hamper children’s academic achievement, social development and long-term health.
But when people must choose, vision care may lose out to more pressing medical concerns, said Block, who was on the committee that developed the report.
“Vision issues are not life-threatening,” she said. “People get through their day knowing they can’t see as well as they’d like.”
Insurance can make regular eye exams, glasses and treatment for medical problems such as cataracts more accessible and affordable. But comprehensive vision coverage is often achieved only through a patchwork of plans.
The Medicare program that provides coverage for millions of Americans age 65 and older doesn’t include routine eye exams, refraction testing or eyeglasses. Some tests are covered if you’re at high risk for a condition such as glaucoma, for example. And if you develop a vision-related medical condition such as cataracts, the program will cover your medical care.
But if you’re just a normal 70-year-old and you want to get your eyes examined, the program won’t cover it, said Dr. David Glasser, an ophthalmologist in Columbia, Md., who is a clinical spokesman for the American Academy of Ophthalmology. If you make an appointment because you’re experiencing troubling symptoms and get measured for eyeglasses while there, you’ll likely be charged anywhere from about $30 to $75, Glasser said.
There are a few exceptions. Medicare will pay for one pair of glasses or contact lenses following cataract surgery, for example. Some Medicare Advantage plans offer vision care.
Many commercial health insurance plans also exclude routine vision care from their coverage. Employers may offer workers a separate vision plan to fill in the gaps.
VSP Vision Care provides vision care plans to 60,000 employers and other clients, said Kate Renwick-Espinosa, the organization’s president. A typical plan provides coverage for a comprehensive eye exam once a year and an allowance toward standard eyeglasses or contact lenses, sometimes with a copayment. Also, individuals seeking plans make up a growing part of their business, she said.
Vision coverage for kids improved under the Affordable Care Act. The law requires most plans sold on the individual and small-group market to offer vision benefits for children younger than 19. That generally means that those plans cover a comprehensive eye exam, including refraction, every year, as well as a pair of glasses or contact lenses.
But since pediatric eye exams aren’t considered preventive care that must be covered without charging people anything out-of-pocket under the ACA, they’re subject to copays and the deductible.
Medicaid programs for low-income people also typically cover vision benefits for children and sometimes for adults as well, said Dr. Christopher Quinn, president of the American Optometric Association, a professional group.
But coverage alone isn’t enough. To bring down the number of people with undiagnosed or uncorrected vision, education is key to helping people understand the importance of eye health in maintaining good vision. Just as important, it can also reduce the impact of chronic conditions such as diabetes, the national academies’ report found.
“All health care providers need to at least ask vision questions when providing primary care,” said Block.
SOURCE:
Andrews M (13 JUNE 2018). "Lack Of Insurance Exposes Blind Spots In Vision Care" [Web Blog Post]. Retrieved from https://khn.org/news/lack-of-insurance-exposes-blind-spots-in-vision-care/
Healthcare analytics market grows as providers take aim at cost-cutting
A combination of artificial and human intelligence data analytics, offering the opportunity to bring greater customization to medical approaches, is expected to increase in demand over the next few years.
 Data-enriched tools have cut the communication gap between caregivers and patients even as they provide a large amount of data that can be used to create personalized treatments. (Image: Shutterstock)
Data-enriched tools have cut the communication gap between caregivers and patients even as they provide a large amount of data that can be used to create personalized treatments. (Image: Shutterstock)
The need by hospitals and other health care providers to cut the cost of providing care is helping to drive up the global health care/analytics market, to reach an anticipated worth of $53.65 billion by 2025.
That’s according to a new report by Grand View Research, Inc., which says that hospitals are already using health care analytics to manage the number of workers working in a particular shift.
Citing the example of a hospital in Paris that uses health care analytics to predict the number of patients that may be hospitalized, the report points out that such data can be used to decide the number of staff members that will be needed for a particular shift, thus assisting in driving down the cost of labor in hospitals.
Data-enriched tools such as mHealth, eHealth, Electronic Health Records and mobile applications have cut the communication gap between caregivers and patients even as they provide a large amount of data that can be used to create personalized treatments. However, patients might hesitate to use such tools; that could weigh on the implementation of analytics.
But a combination of artificial and human intelligence data analytics, offering the opportunity to bring greater customization to medical approaches, is expected to expand demand for such tools over the next few years.
Among other findings in the report is the significant market share held by descriptive analytics in 2015 because of its applications in process optimization in organizations. In addition, the services category dominated the component segment in 2015, with outsourcing of big data services contributing to their growth in aiding the high volume of services rendered.
The hardware systems category came out the winner in the component segment, with the high cost of hardware contributing to its growth, while on-premise delivered analytic services dominated the delivery mode category in 2015, capturing a market share of approximately 54.0 percent.
North America has captured a significant share in the global market, the report finds, with advanced health care infrastructure in the region and growing per capita health care spending supporting greater consumption of these services.
Source:
By Marlene Satter | April 02, 2018 at 12:13 PM | Originally published on BenefitsPro