3 ideas to ease the transition to a high-deductible world
With high-deductible health plans rising, employers may not be thinking about the drastic changes happening in the future. Here are some tips to make a transition into a high deductible industry painless.
We’re all familiar with the necessary evils of today’s society: paying taxes, going to the dentist and sitting in rush-hour traffic. Now, there’s another one to add to the list — high deductible health plans (HDHPs). They’re on the rise due to increasingly unmanageable health care costs caused by factors such as increased carrier and hospital consolidation, unregulated pharmaceutical prices, and a lack of financial awareness among medical providers.
In response, prudent employers who want to continue providing health benefits but can’t keep up with the costs are turning to HDHPs to share the financial burden with employees and encouraging those employees to become more disciplined shoppers. This is predictably being met with resistance.
But there’s a more urgent matter at hand: until we find a way to flip the health-care system on its head, we’re anticipating a future where networks get narrower and significantly limit options and deductibles rise to catastrophic heights.
Employers may not be thinking ahead for these drastic changes, which is why brokers can be instrumental in helping clients guide their employees toward the necessary mental and financial preparations. Here are a few ideas to get them started.
1. Shift gears to plan beyond the calendar year.
For most, health care is an infrequent experience that’s handled reactively: you get sick, you go to the doctor, your insurance foots the bill. However, now that employees are on the hook for potentially thousands of dollars, it’s crucial that they plan ahead.
To facilitate this shift in mindset, employers should encourage employees to:
- Utilize a health savings account (HSA):When it comes to HSAs, people tend to fall into one of two schools of thought: “HSAs are a silver bullet” or “HSAs are a terrible excuse by politicians to allow the existence of HDHPs.” Rarely is a situation so black and white, and this one is no exception. HSAs aren’t the best choice for everyone. Certain demographics can’t afford to juggle the high costs of health care (and life) while also contributing funds to an account. However, it’s important to keep in mind that as costs continue to rise, more people will be pushed above the HSA qualification line and having an account may be the only life raft available when drowning in high deductibles — a trend we’re already starting to see.In an ideal world, the HSA wouldn’t exist. Out-of-control health care costs bear the blame for solutions like HDHPs — and the HSA is our consolation prize. The reason I advocate the utilization of these accounts for long-term planning is because they are the only health care benefit we have that encourages people to think beyond 12 months. Unlike the flexible spending account (FSA), the money in an HSA rolls over every year and grows over time, so it lets people save for years down the road (maybe when the pediatrician bills pile up, or you finally have that major surgery) vs. scrambling to spend their funds before the end of the year. Also, if an employer is contributing to an employee’s HSA, it’s leaving money on the table not to sign up for an account.
- Shop for the best “deals”:Unless someone is a frequent flyer in the health care system, they might brush off shopping for healthcare since it seems like a lot of effort for a single doctor’s visit. However, considering the fact that the cost of an ACL surgery can vary as much as $17,000, those numbers certainly add up over time. (Even more so if a patient fails to find care that’s in network.) Helping employees understand this concept, and pairing it with an easy-to-use transparency solution, can save them tons of money in the long run — especially if the cost savings from each doctor’s visit are deposited into an HSA for future use.
2. Recognize that options are still available.
I’m not going to try to frame high deductibles in a positive light. It’s not the ideal situation for consumers or employers. But sometimes, just knowing there are options in a seemingly bleak situation can provide temporary relief. Here are some tips for employers to share with employees when they’re frustrated about their HDHPs:
- Ask questions:Employees shouldn’t be afraid to ask questions. Healthcare is known for being convoluted, so it’s likely they’re not alone in any confusion they experience. They should start with health insurance and take time with the HR manager to understand the specifics of their coinsurance, copays, deductibles, and benefits so they’re aware of all their options, such as free preventive services. Another great place for questions is at the doctor’s office. Asking about and negotiating costs (yes, you can do that!) can have huge payoffs — Consumer Reports found that only 31 percent of Americans haggle with doctors over medical bills but that 93 percent of those who did were successful, with more than a third of those saving more than $100.
- Stay educated:“Education” can be a tired term for brokers and employers. Employees never seem to read the emails and collateral materials that teams painstakingly curate each year. While disheartening, I think the focus on education is a long but ultimately rewarding process. Consider the 401(k). These plans struggled through the recessions in the early 2000s, but through constant behavioral reinforcement (helped largely by policies such as The Pension Protection Act, which made it easier for companies to automatically enroll their employees in 401(k) plans) and continued efforts by employers, 401(K)s bounced back and hold $4.8 trillion in assets today.The same lesson can be applied to your education efforts as well. That is, eventually the education will stick. So help create a new ecosystem for employees to navigate by getting timely information and resources out there about maximizing HDHPs and utilizing HSAs.
3. Stay optimistic because change is coming.
This point is a bit more abstract. Worrying about health care costs is exhausting, and things are likely to get worse before they get better. However, there’s been a lot of news in the health care space that should bring a glimmer of optimism.
For instance, we heard about the partnering of three industry powerhouses to create a new health care company for their employees. It’s been fascinating to see how much chatter this announcement has already generated and will likely keep traditional employer health care vendors on their toes.
While the trend of employers building coalitions to tackle health care costs is nothing new and it’s too early to tell how successful this initiative will be, the bigger point is that this is a strong signal that change is desperately needed. More and more companies — regardless of what industry they’re in — are starting to realize that they’re all in the business of health care. And as we gain power in numbers, I believe we will build the momentum to create some serious change.
It’s tough to win in today’s health care world, and it’s likely going to get even more challenging over the next few years. But if brokers and employers can provide the right level of guidance, education, and resources, they can help employees better mentally and financially manage their high-deductible futures.
SOURCE:
Vivero, D (2 July 2018) "3 ideas to ease the transition to a high-deductible world" [Web Blog Post]. Retrieved from https://www.benefitspro.com/2018/02/08/3-ideas-to-ease-the-transition-to-a-high-deductibl/
3 Ways to Reshape How You Communicate About Benefits with Millennials
Communicating the benefit needs amongst generations and can cause confusion when keeping up with the satisfaction of your younger employees. Ensure millennial happiness with these tips on their unique benefit standards.
As two millennials ourselves, we know what most people think about Generation Y. Many use terms like “techy,” “entitled” and maybe even “lazy” to describe our generation.
But, the reality is today’s millennials are more global, civic-minded and, though you may not expect it,financially conscious than any other generation. And, according to the Pew Research Center, we now represent 35 percent of today’s workforce.
Millennials are also now getting married and starting families. And yes, purchasing more benefits products through their employers as a result.
As we millennials grow up, it’s important to reconsider how you communicate with us about benefits—because it’s a lot different than how you’ve communicated with other employees in the past.
For example, consider your Gen X and Baby Boomer employees for a moment. When you communicate about benefits with them, it’s relatively straightforward. You probably use tools like email, in-person meetings, flyers and newsletters. And messaging probably revolves around safety, reducing risk and explaining the finer points of the benefits themselves.
But when you’re talking about benefits to millennials, things should be a little different. We’re more digitally fluent than other generations. We’re demanding more flexibility—in our work and family lives. And, we’re increasingly cost-conscious.
It’s a different approach. And, we want to talk about three key ways you can start to reshape how talk with millennials more effectively when it comes to benefits:
For millennials, it’s all about the emotion and sense of responsibility. One of the most interesting findings we’ve picked up over the last few years when communicating with millennials has been to focus messaging on making an emotional connection. Highlight the peace of mind benefits will provide. Discuss the fact that purchasing benefits like disability, life and critical illness insurance through their employer is the right, and responsible, thing to do.
In a recent survey conducted on behalf of Trustmark Voluntary Benefit Solutions “providing peace of mind” was the number one reason millennials gave for why they enrolled in key benefit areas. While this was true across all generations in the study, millennials chose “it’s the responsible thing to do” more than others as a secondary reason for purchase. That emotional connection tied in with responsibility is absolutely key when talking to this demographic.
Millennial stereotypes don’t apply. If you’re communicating with millennials, most people would think digital technologies like text messages and social media would be the way to go. However, that’s not the case. According to Trustmark research, millennials listed “meeting in person” and “calling a representative” as their top preferred channels for communicating during enrollment periods—followed by digital communications channels. Surprising, right? It probably shouldn’t be, given millennials’ desire for more personalization in multiple facets of their lives.
Value, convenience and high-level messaging are key. Through our research, we found that millennials react favorably to messaging around value and convenience—so be sure to hit on those points throughout the enrollment process. For instance, explain why coverage is needed or why an employer-paid policy is not enough. Talk about benefit policy costs in comparison to other low-cost items, like a daily cup of coffee. Discuss the value of employer contributions—and what those contributions can mean to millennials’ bottom lines. Also, make sure to share the convenience and ease of payroll deductions; how their employer is simplifying things by making the deduction and payment for them.
Finally, remember, when it comes to benefits, millennials aren’t as concerned about the details of their insurance plans. They want to understand the basics—what’s covered, how much it costs, and why they might consider a specific offering over another. Resist the urge to focus on the fine print, and keep messaging at the higher levels.
Magic number 3
One more thing that may help reshape your approach to communicating with millennials: The number three. That’s the minimum number of times you should be communicating with millennials during your enrollment process. Our research found that employees remembered and appreciated benefits more when they saw three or more distinct communications. In fact, 72 percent of employees who received three types of benefits communication rate themselves “likely” or “very likely” to recommend their employer based specifically on their benefits program.
Does that help give you some ideas for how to reshape your approach to communicating with millennials about benefits? Overall, just make sure to remember that we millennials are looking for personal and professional offerings from our employers that are unique to us—including benefits. And be sure you’re ready to talk with millennials using the right messaging, the right tools and the right cadence to ensure success.
SOURCE:
Dahlinger, M and Moser, C (27 June 2018) " 3 ways to reshape how you communicate about benefits with millennials" [Web Blog Post]. Retrieved from https://www.benefitspro.com/2018/06/27/3-ways-to-reshape-how-you-communicate-about-benefi/
Quality trumps convenience among employees
Convenience, or quality? Take a look into why researchers are saying quality of a doctors visit outshines convenience when scheduling the next appointment.
Faced with the choice between going to a conveniently located doctor’s office or a more qualified physician, group health plan members are four times more likely to embrace the better-perceived medical professional.
“Traditional metrics like patient ratings, prescribing rates and volume of patients seen were not nearly as compelling to respondents as more qualitative, contextualized statements about a doctor’s clinical expertise,” according to Nate Freese, senior director of data strategy at Grand Rounds, a healthcare service provider for employees in need of local and remote specialty care.
The data is based on a study of 1,100 members covered by Grand Rounds, which is headquartered in San Francisco.
While surprising, Freese says that result depends on the information and messaging that’s provided to employees. Just 14% of respondents based their choice on clinical expertise if they saw traditional physician profiles, whereas it was 69% if they saw contextualized profiles. Contextualized profiles offered more information in complete sentences compared to traditional profiles. These profiles also compared data against other doctors and specialists, such as appointment wait times, expertise and patient satisfaction.
Freese is encouraged by these findings, which were recently presented at the National Healthcare Ratings Summit. “Don’t sell employees short in terms of their ability to appreciate quality and willingness to sacrifice convenience,” he says.
Offering more subjective interpretation of hard quality metrics would be helpful, Freese explains, as long as employers and their advisers are careful not to “overstep what can be reasonably inferred based on available data.”
Another caveat to consider is that finding high quality providers may not be inherently more difficult in narrow networks. Rather, he says, the issue is when health plan members “lack the ability to identify them. And so, it’s more about presenting information in the right way.”
Providing compelling quality information can achieve the same results of a narrow network, he notes. But he hastens to add that even narrow networks must be sufficiently broad enough for members to have a reasonable amount of choice. Geography also plays a role. “You could be in the broadest network, but by virtue of where you live, have reduced choice,” he says.
Michael Hough, executive vice president and U.S. founder of Advance Medical, believes the quality metrics that are currently available are insufficient for several reasons. “We’re looking at things like frequency and whether the outcomes are horrible,” he says. “But just because the outcomes weren’t horrible doesn’t mean they were good, either.” Desired outcomes depend on what’s going on with patients and whether their objectives are being achieved.
The context of care is “extremely important,” Hough explains, noting the importance of relationships between the patient and a trained physician based on human interaction, as well as the delivery of services. Also, while he believes the rise of telemedicine and self-service “is good for many parts of our lives,” Hough cautions that it’s not necessarily true for healthcare because meaningful relationships trump convenience.
SOURCE:
Shutan, B (22 June 2018) "Quality trumps convenience among employees" [Web Blog Post]. Retrieved from https://www.employeebenefitadviser.com/news/quality-trumps-convenience-among-employees?tag=00000151-16d0-def7-a1db-97f0240f0000
How faking your feelings at work can be damaging
Putting up a fake smile on Monday morning is sometimes unavoidable. There could be consequences to carrying a heavy emotional labor load to get over the Monday Blues.
Imagine yourself 35,000 feet up, pushing a trolley down a narrow aisle surrounded by restless passengers. A toddler is blocking your path, his parents not immediately visible. A passenger is irritated that he can no longer pay cash for an in-flight meal, another is demanding to be allowed past to use the toilet. And your job is to meet all of their needs with the same show of friendly willingness.
For a cabin crew member, this is when emotional labour kicks in at work.
A term first coined by sociologist Arlie Hochschild, it’s the work we do to regulate our emotions to create “a publicly visible facial and bodily display within the workplace”.
Simply put, it is the effort that goes into expressing something we don’t genuinely feel. It can go both ways – expressing positivity we don’t feel or suppressing our negative emotions.
Unhelpful attitudes such as ‘I’m not good enough’ may lead to thinking patterns in the workplace such as ‘No-one else is working as hard as I seem to be’ or ‘I must do a perfect job’, and can initiate and maintain high levels of workplace anxiety - Leonard
Hochschild’s initial research focused on the airline industry, but it’s not just in-flight staff keeping up appearances. In fact, experts say emotional labour is a feature of nearly all occupations in which we interact with people, whether we work in a customer-facing role or not. The chances are, wherever you work, you spend a fair portion of your working day doing it.
When research into emotional labour first began, it focused on the service industry with the underlying presumption that the more client or customer interaction you had, the more emotional labour was needed.
However, more recently psychologists have expanded their focus to other professions and found burnout can relate more closely to how employees manage their emotions during interactions, rather than the volume of interactions themselves.
Perhaps this morning you turned to a colleague to convey interest in what they said, or had to work hard not to rise to criticism. It may have been that biting your lip rather than expressing feeling hurt was particularly demanding of your inner resource.
But in some cases maintaining the façade can become too much, and the toll is cumulative. Mira W, who preferred not to give her last name, recently left a job with a top airline based in the Middle East because she felt her mental wellbeing was at stake.
In her last position, the “customer was king”, she says. “I once got called 'whore' because a passenger didn't respond when I asked if he wanted coffee. I’d asked him twice and then moved to the next person. I got a tirade of abuse from the man.”
“When I explained what happened to my senior, I was told I must have said or done something to warrant this response… I was then told I should go and apologise.”
“Sometimes I would have to actively choose my facial expression, for example during severe turbulence or an aborted landing,” she says. “Projecting a calm demeanour is essential to keep others calm. So that aspect didn't worry me. It was more the feeling that I had no voice when treated unfairly or extremely rudely.”
During her time with the airline, she encountered abuse and sexism – and was expected to smile through it. “I was constantly having to hide how I felt.
Over the years and particularly in her last role, handling the stress caused by suppressing her emotions became much harder. Small things seemed huge, she dreaded going to work and her anxiety escalated.
“I felt angry all the time and as if I might lose control and hit someone or just explode and throw something at the next passenger to call me a swear word or touch me. So, I quit,” she says.
She is now seeing a therapist to deal with the emotional fallout. She attributes some of the problems to isolation from family and a brutal travel schedule, but has no doubt that if she hadn’t had to suppress her emotions so much, she might still be in the industry.
Mira is not alone. Across the globe, employees in many professions are expected to embrace a work culture that requires the outward display of particular emotions – these can including ambition, aggression and a hunger for success.
The way we handle emotional labour can be categorised in two ways – surface acting and deep acting
A few years ago, the New York Times wrote a “lengthy piece about the “Amazon Way”,describing very specific and exacting behaviour the retail company required of its employees and the effects, both positive and negative, that this had on some of them. While some appeared to thrive in the environment, others struggled with constant pressure to show the correct corporate face.
“How we cope with high levels of emotional labour likely has its origins in childhood experience, which shapes the attitudes we develop about ourselves, others and the world,” says clinical and occupational psychologist Lucy Leonard.
“Unhelpful attitudes such as ‘I’m not good enough’ may lead to thinking patterns in the workplace such as ‘No-one else is working as hard as I seem to be’ or ‘I must do a perfect job”, and can initiate and maintain high levels of workplace anxiety,” says Leonard.
Workers are often expected to provide good service to people expressing anger or anxiety – and may have to do this while feeling frustrated, worried or offended themselves.
“This continuous regulation of their own emotional expression can result in a reduced sense of self-worth and feeling disconnected from others,” she says.
Hochschild suggests that the way we handle emotional labour can be categorised in two ways – surface acting and deep acting – and that the option we choose can affect the toll it takes on us.
Take the example of a particularly tough phone call. If you are surface acting you respond to the caller by altering your outward expression, saying the appropriate things, listening while keeping your actual feelings entirely intact. With deep acting you make a deliberate effort to change your real feelings to tap in to what the person is saying – you may not agree with the manner of it but appreciate the aim.
Both could be thought of as just being polite but the latter approach – trying to emotionally connect with another person’s point of view – is associated with a lower risk of burnout.
Jennifer George’s role as a liaison nurse with a psychiatric specialism in the Accident & Emergency department at Kings College London Hospital puts her at the sharp end of health care. Every day she must determine patients’ needs – do they genuinely need to be admitted, just want to be looked after for a while or are they seeking access to drugs?
“It’s important to me that I test my own initial assumptions,” she says. “As far as I can, I tap into the story and really listen. It’s my job but it also reduces the stress I take on.”
“Sometimes I’ll have an instinctive sense that the person is trying to deceive, or I can become bored with what they’re saying. But I can’t sit there and dismiss something as fabrication and I don’t want to.”
This process can be upsetting, she says. Sometimes she has to say no “in a very direct way”, and the environment can be noisy and threatening. “I stay as much as I can true to myself and my beliefs. Even though I need to be open to what both fellow professionals and would-be and genuine patient cases say to me, I will not say anything I don’t believe and that I don’t believe to be right. And that helps me,” she says.
When things get tough, she talks to colleagues to unload. “It’s the saying it out loud that allows me to test and validate my own reaction. I can then go back to the person concerned,” she says.
Ruth Hargrove, a former trial lawyer based in California, also faces tricky interactions in her work representing San Diego students pro bono in disciplinary matters. “Pretty much everyone you are dealing with in the system can make you labour emotionally,” she says.
One problem, says Hargrove, is that some lawyers will launch personal attacks based on any perceived weakness – gender, youth – rather than focusing on the actual issues of the case.
“I have dealt with it catastrophically in the past and let it eat at my self-esteem,” she says. “But when I do it right, I realise that I can separate myself out from it and see that [their attack] is evidence of their weakness.”
Rather than refuting specific, personal allegations, she simply sends back a one-line email saying she disagrees. “Not rising to things is huge,” she says. “It’s a disinclination to engage in the emotional battle that someone else wants you to engage in. I keep in sight the real work that needs to be done.”
Those who report regularly having to display emotions at work that conflict with their own feelings are more likely to experience emotional exhaustion
Hargrove also has to deal with the expectations of clients who believe – sometimes unrealistically – that if they have been wronged, justice will prevail. She understands their feelings, even as she has to set them straight.
“I empathise here, as a parent, with their thought that there should be a remedy, even when I know it’s not going to be achievable. It helps me that this feeling is also true to me.”
Remaining true to your feelings appears to be key – numerous studies show those who report regularly having to display emotions at work that conflict with their own feelings are more likely to experience emotional exhaustion.
Of course, everybody needs to be professional at work and handling difficult clients and colleagues is often just part of the job. But what’s clear is that putting yourself in their shoes and trying to understand their position is ultimately of greater benefit to your own well-being than voicing sentiments that, deep down, you don’t believe.
Leonard says there are steps individuals and organisations can take to prevent burnout. Limiting overtime, taking regular breaks and tackling conflict with colleagues through the right channels early on can help, she says, as can staying healthy and having a fulfilling life outside work. A “climate of authenticity” at work can be beneficial.
“Organizations which allow people to take a break from high levels of emotional regulation and acknowledge their true feelings with understanding and non-judgemental colleagues behind the scenes tend to fare better in the face of these demands,” she says.
Such a climate can also foster better empathy, she adds, by allowing workers to maintain emotional separation from those with whom they must interact.
Where it is possible, workers should be truly empathetic, be aware of the impact the interaction is having on them and try to communicate in an authentic way. This, she says, can “protect you from communicating in a disingenuous manner and then feeling exhausted by your efforts and resentful of having to fake it”.
SOURCE:
Levy, K (25 June 2018) "How faking your feelings at work can be damaging" [Web Blog Post]. Retrieved from https://www.bbc.com/capital/story/20180619-why-suppressing-anger-at-work-is-bad
3 questions advisers should ask about the potential CVS-Aetna deal
In a rapid changing market, stay ahead of the curve by asking these three questions on the potential CVS-Aetna deal to help determine how it will impact the health insurance industry.
The news that CVS has reportedly launched a $66 billion bid to buy Aetna shows that once unimaginable mergers are becoming the norm. But it also raises some important questions for brokers about the future of group benefits, and how to operate in a fast-moving and constantly changing landscape.
Here are three questions to ask when determining how this potential business deal will impact the employer-based health insurance market:
1) Will this move give Aetna a competitive advantage in the group space?
How are other carriers going to feel about having to compete with an insurer that has pharmacy data on the majority of Americans? Anthem may be at the top of the list with worries, as the company just last week announced that it will partner with CVS to launch its own pharmacy benefits manager called IngenioRx.
2) Are healthcare companies too focused on M&A?
A year ago, Aetna was trying to acquire Humana, and Anthem was trying to buy Cigna. Brokers everywhere were concerned about carrier consolidation and what a lack of competition would do to group prices. How have things pivoted to pharmacy so quickly?
The CVS deal may represent gains for both parties. The deal would give Aetna a new avenue for business growth, and CVS would gain some much needed ground against Amazon’s rumored entrance into the drug business.
But what does this emphasis on inorganic, M&A growth say about the healthcare industry? Healthcare consolidation has been a trend for years, but it hasn’t always worked in consumers’ favor, which could leave brokers wary of this deal.
3) Why should employers care?
What impact will this deal have on prescription prices for employers? Prescription drug costs are one of the largest drivers of employer healthcare spend, so the question is critical. Will Aetna and CVS be able to improve efficiencies and lower costs, or monopolize their group markets?
Another point of interest for employers is the possibility of narrowed prescription options. With narrowing provider networks becoming standard, this deal could result in limited consumer options when it comes to prescription drugs.
On the other hand, the deal could spark cost-saving changes in healthcare delivery. It’s not hard to imagine CVS augmenting their MinuteClinic operations with Aetna’s volume.
Employees might find they like having retail access to primary care at a lower price point, with after-hours service, easy-to book appointments, and pharmacy services built right in. This partnership may be the push retail healthcare needs to become a cornerstone of the primary care model.
SOURCE:
Tolbert, B (22 June 2018) "3 questions advisers should ask about the potential CVS-Aetna deal" [Web Blog Post]. Retrieved from https://www.employeebenefitadviser.com/opinion/3-questions-advisers-should-ask-about-the-potential-cvs-aetna-merger
Five steps to becoming a trusted retirement plan adviser
Discover creative ways to deliver the best retirement plan to your employees with these five steps in retirement plan advising.
Many trends within the employee benefits industry challenge advisers to think creatively on behalf of their clients. For instance, millennials are more likely to pay off student loans and less likely to contribute to their company’s 401(k) plan. They lose the benefit of compound interest over all those years to retirement, which over decades, can amount to up to 80% of a millennial’s nest egg.
When companies experience low participation rates with new hires, the overall health of the plan will suffer and many of the more highly compensated and key employees may not be able to defer as much as they would like into the plan. Advisers must develop relationships with business owners to establish customized retirement plans that work best for their and their employees’ needs.
When advisers overcome these challenges they expand their client base and move toward success. The following five steps will help retirement plan advisers bring their career to the next level:
Understand the fiduciary requirements and minimize the risk of the employer
Strive to impart knowledge on the employer and the participants to make them confident in their retirement plans. Company owners will feel more comfortable if an adviser helps to reduce the fiduciary risk associated with the creation and ongoing operation of a plan. Advisers can share and even take over most of the fiduciary responsibility with the employer to lessen the pressure. With the right information, a business owner can understand the requirements of the plan and is motivated to establish a 401(k) or other type of plan for the benefit of their employees and overall business objectives.
Know the best plan options for the companies you’re serving
Not every company should have a 401(k) plan. While 401(k) plans may be optimal for large and even small companies, small companies may benefit from other types of plans. Small businesses often operate at a loss or minimal profit for many years before they generate significant profit. As a result, business owners may seek a plan — such as a defined benefit plan — that allows them to contribute more toward their retirement. In some cases, this may more than triple the amount of yearly contributions an employer can make compared to a 401(k) plan. Employers can contribute to a defined benefit plan and take a tax deduction equivalent to the contributions made to the plan.
Understand the tax advantages of retirement plans
Successful plan advisers should understand the tax advantages associated with the chosen retirement plan for both the owners and the participants. Traditional 401(k) plans tend to provide the most benefits to employees with tax-deferred contributions. On the other hand, small company owners can benefit from the tax advantages of properly designed cash balance or defined benefit plans. These frequently overlooked plans enable employers to deduct the cost of the company’s plan from their taxable income to secure tax savings.
Employee benefit advisers must have this foundational understanding of the tax advantages to successfully serve their clients. Partner with a retirement company record-keeper and a third-party administrator to learn the details for each option.
Discover profitable prospects among small companies too
Many employee benefit advisers in search of success avoid talking to small companies. However, these small companies have significant potential and are vital to success in an otherwise crowded market. Small companies, even with only three to five employees, are great to work with, especially if you help them establish a defined benefit plan, and if it’s the best plan for them. Through these plans, retirement plan advisers can receive the fees needed to provide the service because the company is making larger contributions than to a profit sharing or 401(k) plan.
Target underserved, yet vibrant markets
According to a recent study from the Pew Charitable Trusts, only 53% of small to midsize companies have retirement plans in place. Owners may think they are too small to be able to afford and monitor a program. These businesses are important prospects to pursue. Make yourself known to these companies and show the employer that there is a retirement plan that will work for their employees and company, no matter the size. Explain what program the company can implement and easily administer with your guidance.
Small companies provide great opportunities for advisers to become successful and differentiate themselves from other industry professionals. Keep in mind that these small companies are also more dependent on advisers because of the costs and risk associated with retirement plans. They will require more frequent contact for advice and personalized service. If you do not have the right expertise in the beginning, partner with someone in your office or a TPA until you have the credentials and knowledge to advise small companies on your own.
SOURCE:
Weintraub, M (19 June 2018) "Five steps to becoming a trusted retirement plan adviser" [Web Blog Post]. Retrieved from https://www.employeebenefitadviser.com/opinion/five-steps-to-becoming-a-trusted-retirement-plan-adviser?brief=00000152-146e-d1cc-a5fa-7cff8fee0000
7 wellness program ideas you may want to steal
Need more energy and excitement in your office? Keep your employees healthy and motivated with these fun wellness program ideas.
Building your own workplace wellness program takes work–and time–but it’s worth it.
“It’s an investment we need to make,” Jennifer Bartlett, HR director at Griffin Communication, told a group of benefits managers during a session at the Human Resource Executive Health and Benefits Leadership Conference. “We want [employees] to be healthy and happy, and if they’re healthy and happy they’ll be more productive.”
Bartlett shared her experiences building, and (continually) tweaking, a wellness program at her company–a multimedia company running TV outlets across Oklahoma –over the last seven years. “If there was a contest or challenge we’ve done it,” she said, noting there have been some failed ventures.
“We got into wellness because we wanted to reduce health costs, but that’s not why we do it today,” she said. “We do it today because employees like it and it increases morale and engagement.”
Though Griffin Communication's wellness program is extensive and covers more than this list, here are some components of it that's working out well that your company might want to steal:
- Fitbit challenge.Yes, fit bits can make a difference, Bartlett said. The way she implemented a program was to have a handful of goals and different levels as not everyone is at the same pace-some might walk 20,000 steps in a day, while someone else might strive for 5,000. There are also competition and rewards attached. At Griffin Communications, the company purchased a number of Fitbits, then sold them to its employees for half the cost.
- Race entry.Griffin tries to get its employees moving by being supportive of their fitness goals. If an employee wants to participate in a race-whether walking or running a 5k or even a marathon, it will reimburse them up to $50 one time.
- Wellness pantry.This idea, Bartlett said, was "more popular than I ever could have imagined." Bartlett stocks up the fridge and pantry in the company's kitchen with healthy food options. Employees then pay whole sale the price of the food, so it's a cheap option for them to instead of hitting the vending machine. "Employees can pay 25 cents for a bottled water or $1.50 for a soda from the machine."
- Gym membership."We don't have an onsite workout facility, but we offer 50 percent reimbursement of (employees') gym membership cost up to a max of 200 per year," she said. The company also reimburses employees for fitness classes, such as yoga.
- Biggest Loser contest.Though this contest isn't always popular among companies, a Biggest Loser-type competition- in which employees compete to lose the most weight-worked out well at Griffin. Plus, Bartlett said, "this doesn't cost us anything because the employee buys in $10 to do it." She also insisted the company is sensitive to employees. For example, they only share percentages of weight loss instead of sharing how much each worker weights.
- "Project Zero" contest.This is a program pretty much everyone can use: Its aim is to avoid gaining the dreaded holiday wights. The contest runs from early to mid- November through the first of the year. "Participants will weigh in the first and last day of the contest," Bartlett said. "The goal is to not gain weight during the holidays-we're not trying to get people to lose weight but we're just to not get them to not eat that third piece of pie."
- Corporate challenges.Nothing both builds camaraderie and encourages fitness like a team sports or company field day. Bartlett said that employees have basically taken this idea and run with it themselves- coming up with fun ideas throughout the year.
SOURCE:
Mayer K (14 June 2018) "7 wellness program ideas you may want to steal" [Web Blog Post]. Retrieved from https://www.benefitspro.com/2015/10/10/7-wellness-program-ideas-you-may-want-to-steal/
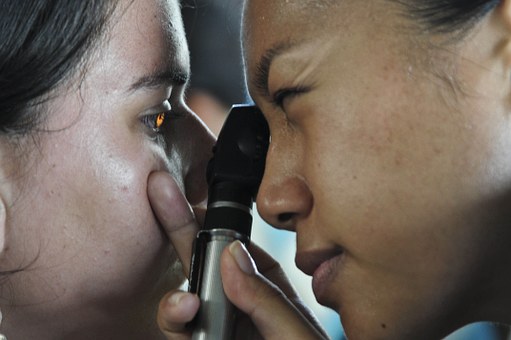
Lack Of Insurance Exposes Blind Spots In Vision Care
Vision problems are typically not life threatening but can impact the success of your everyday life. Vision care is a significant benefit that could change the lives of many families.
Every day, a school bus drops off as many as 45 children at a community eye clinic on Chicago’s South Side. Many of them are referred to the clinic after failing vision screenings at their public schools.
Clinicians and students from the Illinois College of Optometry give the children comprehensive eye exams, which feature refraction tests to determine a correct prescription for eyeglasses and dilation of their pupils to examine their eyes, including the optic nerve and retina.
No family pays out-of-pocket for the exam. The program bills insurance if the children have coverage, but about a third are uninsured. Operated in partnership with Chicago public schools, the program annually serves up to 7,000 children from birth through high school.
“Many of the kids we’re serving fall through the cracks,” said Dr. Sandra Block, a professor of optometry at the Illinois College of Optometry and medical director of the school-based vision clinics program. Many are low-income Hispanic and African-American children whose parents may not speak English or are immigrants who are not in the country legally.
Falling through the cracks is not an uncommon problem when it comes to vision care. According to a 2016 report from the National Academies of Sciences, Engineering and Medicine, as many as 16 million people in the United States have undiagnosed or uncorrected “refractive” errors that could be fixed with eyeglasses, contact lenses or surgery. And while insurance coverage for eye exams and corrective lenses clearly has improved, significant gaps remain.
The national academies’ report noted that impaired vision affects how people experience their world, including normal communication and social activities, independence and mobility. Not seeing clearly can hamper children’s academic achievement, social development and long-term health.
But when people must choose, vision care may lose out to more pressing medical concerns, said Block, who was on the committee that developed the report.
“Vision issues are not life-threatening,” she said. “People get through their day knowing they can’t see as well as they’d like.”
Insurance can make regular eye exams, glasses and treatment for medical problems such as cataracts more accessible and affordable. But comprehensive vision coverage is often achieved only through a patchwork of plans.
The Medicare program that provides coverage for millions of Americans age 65 and older doesn’t include routine eye exams, refraction testing or eyeglasses. Some tests are covered if you’re at high risk for a condition such as glaucoma, for example. And if you develop a vision-related medical condition such as cataracts, the program will cover your medical care.
But if you’re just a normal 70-year-old and you want to get your eyes examined, the program won’t cover it, said Dr. David Glasser, an ophthalmologist in Columbia, Md., who is a clinical spokesman for the American Academy of Ophthalmology. If you make an appointment because you’re experiencing troubling symptoms and get measured for eyeglasses while there, you’ll likely be charged anywhere from about $30 to $75, Glasser said.
There are a few exceptions. Medicare will pay for one pair of glasses or contact lenses following cataract surgery, for example. Some Medicare Advantage plans offer vision care.
Many commercial health insurance plans also exclude routine vision care from their coverage. Employers may offer workers a separate vision plan to fill in the gaps.
VSP Vision Care provides vision care plans to 60,000 employers and other clients, said Kate Renwick-Espinosa, the organization’s president. A typical plan provides coverage for a comprehensive eye exam once a year and an allowance toward standard eyeglasses or contact lenses, sometimes with a copayment. Also, individuals seeking plans make up a growing part of their business, she said.
Vision coverage for kids improved under the Affordable Care Act. The law requires most plans sold on the individual and small-group market to offer vision benefits for children younger than 19. That generally means that those plans cover a comprehensive eye exam, including refraction, every year, as well as a pair of glasses or contact lenses.
But since pediatric eye exams aren’t considered preventive care that must be covered without charging people anything out-of-pocket under the ACA, they’re subject to copays and the deductible.
Medicaid programs for low-income people also typically cover vision benefits for children and sometimes for adults as well, said Dr. Christopher Quinn, president of the American Optometric Association, a professional group.
But coverage alone isn’t enough. To bring down the number of people with undiagnosed or uncorrected vision, education is key to helping people understand the importance of eye health in maintaining good vision. Just as important, it can also reduce the impact of chronic conditions such as diabetes, the national academies’ report found.
“All health care providers need to at least ask vision questions when providing primary care,” said Block.
SOURCE:
Andrews M (13 JUNE 2018). "Lack Of Insurance Exposes Blind Spots In Vision Care" [Web Blog Post]. Retrieved from https://khn.org/news/lack-of-insurance-exposes-blind-spots-in-vision-care/
Are You And Your Primary Care Doc Ready To Talk About Your DNA?
Knowing your genes could save your life, especially if a genetic mutation is hereditary. See why incorporating DNA testing is a crucial part of your primary care.
If you have a genetic mutation that increases your risk for a treatable medical condition, would you want to know? For many people the answer is yes. But such information is not commonly part of routine primary care.
For patients at Geisinger Health System, that could soon change. Starting in the next month or so, the Pennsylvania-based system will offer DNA sequencing to 1,000 patients, with the goal to eventually extend the offer to all 3 million Geisinger patients.
The test will look for mutations in at least 77 genes that are associated with dozens of medical conditions ranging from heart disease to cancer, as well as variability in how people respond to pharmaceuticals based on heredity.
“We’re giving more precision to the very important decisions that people need to make,” said Dr. David Feinberg, Geisinger’s president and CEO. In the same way that primary care providers currently suggest checking someone’s cholesterol, “we would have that discussion with patients,” he said. “‘It looks like we haven’t done your genome. Why don’t we do that?’”
Some physicians and health policy analysts question whether such genetic information is necessary to provide good primary care — or feasible for many primary care physicians.
The new clinical program builds on a research biobank and genome-sequencing initiative called MyCode that Geisinger started in 2007 to collect and analyze its patients’ DNA. That effort has enrolled more than 200,000 people.
Like MyCode, the new clinical program is based on whole “exome” sequencing, analyzing the roughly 1 percent of the genome that provides instructions for making proteins, where most known disease-causing mutations occur.
Using this analysis, clinicians might be able to tell Geisinger patients that they have a genetic variant associated with Lynch syndrome, for example, which leads to increased risk of colon and other cancers, or familial hypercholesterolemia, which can result in high cholesterol levels and heart disease at a young age. Some people might learn they have increased susceptibility to malignant hyperthermia, a hereditary mutation that can be fatal since it causes a severe reaction to certain medications used during anesthesia.
Samples of a patient’s blood or spit are used to provide a DNA sample. After analysis, the results are sent to the patient’s primary care doctor.
Before speaking with the patient, the doctor takes a 30-minute online continuing education tutorial to review details about genetic testing and the disorder. Then the patient is informed and invited to meet with the primary care provider, along with a genetic counselor if desired. At that point, doctor and patient can discuss treatment and prevention options, including lifestyle changes like diet and exercise that can reduce the risk of disease.
About 3.5 percent of the people who’ve been tested through Geisinger’s research program had a genetic variant that could result in a medical problem for which clinicians can recommend steps to influence their health, Feinberg said. Only actionable mutations are communicated to patients. Geisinger won’t inform them if they have a variant of the APOE gene that increases their risk for Alzheimer’s disease, for example, because there’s no clinical treatment. (Geisinger is working toward developing a policy for how to handle these results if patients ask for them.)
Wendy Wilson, a Geisinger spokeswoman, said that what they’re doing is very different from direct-to-consumer services like 23andMe, which tests customers’ saliva to determine their genetic risk for several diseases and traits and makes the results available in an online report.
“Geisinger is prescribing DNA sequencing to patients and putting DNA results in electronic health records and actually creating an action plan to prevent that predisposition from occurring. We are preventing disease from happening,” she said.
Geisinger will absorb the estimated $300 to $500 cost of the sequencing test. Insurance companies typically don’t cover DNA sequencing and limit coverage for adult genetic tests for specific mutations, such as those related to the breast cancer susceptibility genes BRCA1 or BRCA2, unless the patient has a family history of the condition or other indications they’re at high risk.
“Most of the medical spending in America is done after people have gotten sick,” said Feinberg. “We think this will decrease spending on a lot of care.”
Some clinicians aren’t so sure. Dr. H. Gilbert Welch is a professor at the Dartmouth Institute for Health Policy and Clinical Practice who has authored books about overdiagnosis and overscreening, including “Less Medicine, More Health.”
He credited Geisinger with carefully targeting the genes in which it looks for actionable mutations instead of taking an all-encompassing approach. He acknowledged that for some conditions, like Lynch syndrome, people with genetic mutations would benefit from being followed closely. But he questioned the value of DNA sequencing to identify other conditions, such as some related to heart disease.
“What are we really going to do differently for those patients?” he asked. “We should all be concerned about heart disease. We should all exercise, we should eat real food.”
Welch said he was also concerned about the cascading effect of expensive and potentially harmful medical treatment when a genetic risk is identified.
“Doctors will feel the pressure to do something: start a medication, order a test, make a referral. You have to be careful. Bad things happen,” he said.
Other clinicians question primary care physicians’ comfort with and time for incorporating DNA sequencing into their practices.
A survey of nearly 500 primary care providers in the New York City area published in Health Affairs this month found that only a third of them had ordered a genetic test, given patients a genetic test result or referred one for genetic counseling in the past year.
Only a quarter of survey respondents said they felt prepared to work with patients who had genetic testing for common diseases or were at high risk for genetic conditions. Just 14 percent reported they were confident they could interpret genetic test results.
“Even though they had training, they felt unprepared to incorporate genomics into their practice,” said Dr. Carol Horowitz, a professor at the Icahn School of Medicine at Mount Sinai in New York, who co-authored the study.
Speaking as a busy primary care practitioner, she questioned the feasibility of adding genomic medicine to regular visits.
“Geisinger is a very well-resourced health system and they’ve made a decision to incorporate that into their practices,” she said. In Harlem, where Horowitz works as an internist, it could be a daunting challenge. “Our plates are already overflowing, and now you’re going to dump a lot more on our plate.”
SOURCE:
Andrews, M (12 June 2018). "Are You And Your Primary Care Doc Ready To Talk About Your DNA?" [Web Blog Post]. Retrieved from https://khn.org/news/are-you-and-your-primary-care-doc-ready-to-talk-about-your-dna/
Viewpoint: Coaching Your Employees to Finish Strong as They Near Retirement
10,000 people a day are retiring. Help your employees transition into retirement with these important strategies.
Baby Boomers are beginning to retire in large numbers. AARP says 10,000 people a day are retiring from work. Most companies have no formal program to aid these employees in this transition. Although we often have extensive onboarding programs, little to nothing is done when an employee is ending his or her career, except a goodbye party.
For many people, upcoming retirement means coasting until the day they are done. Dave was a senior-level manager who announced his retirement one year in advance. The problem was that Dave then became "retired on the job." He stopped innovating. He stopped moving new ideas forward. He avoided conflict by ignoring problems. He no longer aggressively led his team.
Dave had been very successful in his career but he ended poorly, so that was how everyone remembered him. His team suffered poor morale because its members felt they were stuck until Dave left his position. That is a problem for the whole company.
Help retiring employees to end strong at your company. Instead of letting employees coast and drain the company coffers, HR can support retiring workers as they end their careers in the best way possible, fully contributing up until the last day.
Some key strategies include:
- Creating a planning-to-retire educational program.HR should develop a workshop to show employees how to plan out their future, paying special consideration to how they will handle all the free time they will have once they leave the company. The course can cover financial planning, too. The employee will be grateful for this assistance.
- Coaching the employee's manager.Managers of departing employees need instruction on how to support someone leaving the group. The formal coaching should offer proven strategies to keep the employee engaged until his or her last day. The supervisor should encourage the employee to complete as many key projects as possible and accept the responsibility to not let the employee become retired on the job.
- Documenting their knowledge.As many Baby Boomers walk out the door, their depth of experience and insight depart with them. Companies should have these employees document their knowledge by creating a training manual or by adding pages to the organization's intranet so other employees can learn from these folks.
- Training a new employee.Ideally, the organization should promote or hire a replacement and have the departing employee train the new person. Having a two- to three-week training period helps the new employee get up to speed and be more productive, more quickly.
- Offering a "bridge job."Finding talented workers to replace departing Baby Boomers will become harder to do in our tight labor market. Developing a transitional or bridge job where the employee remains at work on a part-time basis may allow the company to avoid the quest for talent that is often not available. Baby Boomers want more flexibility and fewer work hours at the end of their career. In fact, 72 percent say they plan to work in their retirement. Annette was an IT specialist who wanted to leave the energy utility she worked for. The HR department was under the gun to deliver a new human resource information system and asked her to continue working three days a week with the ability to take more unpaid vacations. This new bridge job kept her in her role for 18 months until the big project was completed.
Final days may be a bittersweet time for employees to say goodbye to their co-workers, friends and the company itself. Having a supportive send-off is a great policy to ensure that everyone leaves on a positive note and will speak highly of your organization after the departure.
SOURCE:
Ryan R (4 June 2018) "Viewpoint: Coaching Your Employees to Finish Strong as They Near Retirement" [Web Blog Post]. Retrieved from https://www.shrm.org/ResourcesAndTools/hr-topics/benefits/Pages/Viewpoint-Coaching-Your-Employees-on-Finishing-Strong-As-They-Retire-.aspx?_ga=2.37756515.1310386699.1527610160-238825258.1527610159